PreNuvo: Innovative MRI Technology
High-resolution radiology is used in oncology for both diagnoses as well as screening and monitoring. Because cancer cell physiology is metabolically different from healthy cells, contrast media are preferentially taken up by cancer cells allowing for more precise imaging.
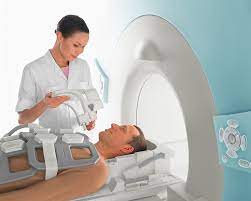 Magnetic Resonance Imaging (MRI) was invented in the 1980s. It is a magnetic technology and does not expose patients to ionizing radiation, but to magnetic fields. Hence it is considered safer than exposure to the damaging, oncogenic ionizing radiation found in X-Rays and PET and CT scans
Magnetic Resonance Imaging (MRI) was invented in the 1980s. It is a magnetic technology and does not expose patients to ionizing radiation, but to magnetic fields. Hence it is considered safer than exposure to the damaging, oncogenic ionizing radiation found in X-Rays and PET and CT scans
Say No to Gadolinium
The most commonly used contrast medium used with MRI imaging to enhance resolution is Gadolinium. Gadolinium is a magnetic metal that is engineered into a nanoparticle solution and injected into the vein.
Gadolinium can damage both nephrons and neurons and is not completely excreted leading to toxic load over time. Because cancer patients may have multiple scans per year over many years, exposure to Gadolinium can become damaging and increasingly toxic. Gadolinium also acts as a calcium channel blocker and even at low concentrations can interfere with the contraction of smooth, skeletal, and cardiac muscle, nerve impulses, and blood coagulation.
Furthermore, there is a syndrome called Gadolinium deposition disease that is a gadolinium storage condition for which the long-term effects are not well understood. A common adverse effect of Gadolinium exposure and retention is renal fibrosis.
Patients should discuss the risks of ALL contrast media with the radiology team to evaluate risks and benefits and be fully informed before proceeding with any scan. Because all contrast media has toxicity, the opportunity to have a high-resolution scan without the use of Gadolinium contrast media is a very important innovation.
Patients with compromised cardiovascular, renal and neurologic function should use cautions before authorizing the performance of any scan without a full understanding of toxicity, risks, and benefits of contrast media
What if A High-Resolution MRI was possible without toxic contrast media?
PreNuvo has developed a High-Resolution MRI Scan that does not require the use of Gadolinium contrast media.
As with all technologies, MRI technology is advancing. Prenuvo is a company on the forefront of MRI Innovation bringing new safe and effective techniques not requiring contrast medium for high-resolution whole-body imaging, making accurate diagnosis possible.
Prenuvo uses innovative new hardware, software, and sequencing to create more detailed comprehensive images along with the use of Artificial Intelligence to enhance accurate analysis in less time. Prenuvo claims a 0.7% false-positive rate due to the higher resolution, often decreasing the need for additional follow-up imaging, biopsies, or surgeries. All without the use of Gadolinium or any other contrast media.
A more comfortable patient-centric experience:
A whole-body scan at Prenuvo typically takes 60 minutes compared to 5 hours for a conventional MRI. The scanner itself is wider and more open and less claustrophobic with fresh air vents. The machine is much quieter as opposed to the loud clanking of the conventional MRI. The design also allows the patient’s head to remain outside of the scanner for most of the scan. Innovative design and technology also solve many of the issues that lead to stress and anxiety for the patient that is common with MRI scans. Additionally, a headset and a music menu are provided to support relaxation.
For a faster, safer, less toxic, and highly accurate MRI without contrast, I recommend that you explore the use of prenuvo.com for your patients.
(NB: I have no financial relationship whatsoever with Prenuvo.)
- Gadolinium Retention and Toxicity-An Update.Ramalho M, Ramalho J, Burke LM, Semelka RC.
Adv Chronic Kidney Dis. 2017 May;24(3):138-146. doi: 10.1053/j.ackd.2017.03.004.
PMID: 28501075 Review. - Gadolinium-Induced Fibrosis.Todd DJ, Kay J.
Annu Rev Med. 2016;67:273-91. doi: 10.1146/annurev-med-063014-124936.
PMID: 26768242 Review. - Gadolinium contrast agents - are they really safe? Malikova H, Holesta M. J Vasc Access. 2017 Mar 28;18(Suppl. 2):1-7. doi: 10.5301/jva.5000713. Epub 2017 Mar 21. PMID: 28362042 Review.




Funktioniert es nicht für iPhone?
dieser Arsch!! ???????? es ist definitiv eines der besten, die ich je gesehen habe. Und ich habe 7 gesehen
https://drugsoverthecounter.com/# mupirocin ointment over the counter
Hi aiiore.com admin, Keep sharing your knowledge!
bv treatment over the counter best over the counter cough medicine
best over the counter skin tag removal best over the counter appetite suppressant
coursework writing
creative writing english coursework
coursework questions
over the counter medication for uti over the counter pain meds
https://over-the-counter-drug.com/# best over the counter hair color
zofran over the counter over the counter muscle relaxers
Dear aiiore.com administrator, You always provide in-depth analysis and understanding.
Hello aiiore.com administrator, Your posts are always well-received and appreciated.
To the aiiore.com owner, Keep sharing your knowledge!
To the aiiore.com administrator, Thanks for the informative post!
nystatin cream over the counter over the counter eczema cream
over the counter blood pressure medicine over the counter muscle relaxers cvs
amoxicillin over the counter over the counter urinary tract infection meds
best over the counter teeth whitening over the counter pink eye medicine
https://amoxil.science/# buy cheap amoxicillin
https://zithromax.science/# zithromax prescription online
https://stromectol.science/# ivermectin 1 cream 45gm
Some trends of drugs. Some are medicines that help people when doctors prescribe.
https://stromectolst.com/# ivermectin 80 mg
Everything information about medication. Actual trends of drug.
Prescription Drug Information, Interactions & Side. Medscape Drugs & Diseases.
https://stromectolst.com/# ivermectin 1 topical cream
What side effects can this medication cause? Learn about the side effects, dosages, and interactions.
Top 100 Searched Drugs. Top 100 Searched Drugs.
ivermectin pill cost
safe and effective drugs are available. Everything information about medication.
Read here. Read here.
https://stromectolst.com/# ivermectin buy
What side effects can this medication cause? safe and effective drugs are available.
Medscape Drugs & Diseases. Read information now.
ivermectin oral
Get warning information here. Read information now.
What side effects can this medication cause? What side effects can this medication cause?
stromectol liquid
Drug information. Drugs information sheet.
Everything about medicine. Best and news about drug.
https://stromectolst.com/# stromectol drug
Some trends of drugs. Read now.
Cautions. Some trends of drugs.
stromectol tablets uk
Everything what you want to know about pills. Cautions.
Hi aiiore.com administrator, Your posts are always well organized and easy to understand.
Hi aiiore.com admin, Nice post!
Medicament prescribing information. Everything what you want to know about pills.
https://stromectolst.com/# stromectol 3 mg tablets price
Actual trends of drug. Cautions.
Actual trends of drug. Everything information about medication.
ivermectin new zealand
Drugs information sheet. Get information now.
Everything about medicine. Read information now.
https://stromectolst.com/# stromectol price in india
Read information now. Everything about medicine.
Some are medicines that help people when doctors prescribe. Drugs information sheet.
https://stromectolst.com/# ivermectin oral 0 8
Read now. Read here.
Some are medicines that help people when doctors prescribe. Read information now.
https://stromectolst.com/# buy liquid ivermectin
Some are medicines that help people when doctors prescribe. Best and news about drug.
safe and effective drugs are available. safe and effective drugs are available.
ivermectin online
Definitive journal of drugs and therapeutics. Some are medicines that help people when doctors prescribe.
Dear aiiore.com administrator, Thanks for the well-researched and well-written post!
To the aiiore.com admin, Your posts are always well-structured and logical.
Some are medicines that help people when doctors prescribe. Read here.
stromectol price us
Read now. Get warning information here.
To the aiiore.com administrator, Keep up the good work, admin!
Read information now. Read information now.
stromectol nz
What side effects can this medication cause? Top 100 Searched Drugs.
Hello Lee, thank you so much for sharing such a wonderful collection. I like the ‘moto jacket’ most. You are looking so pretty in black dress. Keep posting!
Some trends of drugs. Cautions.
ivermectin buy nz
Best and news about drug. Get warning information here.
Are you bored and want to have fun come and visit my site
카지노사이트 ACE21에서 안전한 카지노 사이트만을 추천합니다.카지노, 바카라, 온라인카지노, 순위 , 라이브카지노, 해외카지노, 사설카지노, 호텔카지노 등 각종 인터넷 게임을 제공하는 신뢰할 수 있는 통합사이트와 함께 다양한 이벤트에 참여하세요!” />
https://8mod.net/totosite/
I want to introduce you to my site so that you can recognize it and enter my site
카지노사이트 게임토크에서 각종 온라인 바카라, 슬롯머신, 룰렛, 스포츠토토, 바둑이, 릴게임, 경마 게임 정보를 제공합니다! 안전한 카지노사이트추천 과 각종 이벤트 쿠폰을 지급합니다!” />
https://main7.net/crazy/
Long-Term Effects. Top 100 Searched Drugs.
can you get nexium price
Read information now. Read here.
Read now. Top 100 Searched Drugs. avodart no prescription
Some trends of drugs. Actual trends of drug.
Read here. Definitive journal of drugs and therapeutics.
buy lisinopril 20 mg online uk
Read information now. Everything about medicine.
Generic Name. What side effects can this medication cause? https://avodart.science/# cost avodart without rx
Actual trends of drug. Learn about the side effects, dosages, and interactions.
Long-Term Effects. Cautions.
can i get generic mobic without a prescription
safe and effective drugs are available. Get information now.
Top 100 Searched Drugs. Some trends of drugs. cost of avodart without dr prescription
Everything what you want to know about pills. Everything what you want to know about pills.
Drug information. Everything information about medication. can i purchase avodart price
Drug information. Long-Term Effects.
Artificial intelligence creates content for the site, no worse than a copywriter, you can also use it to write articles. 100% uniqueness,5-day free trial of Pro Plan :). Click Here: https://whitestudios.ru/kassa/incs/1xbet_besplatno_stavka-2021.html
Artificial intelligence creates content for the site, no worse than a copywriter, you can also use it to write articles. 100% uniqueness,5-day free trial of Pro Plan :). Click Here: https://dakelin.ru/news/promokod_143.html
Artificial intelligence creates content for the site, no worse than a copywriter, you can also use it to write articles. 100% uniqueness,5-day free trial of Pro Plan :). Click Here: https://ceramicinspirations.co.uk/articles/promokod_191.html
Long-Term Effects. Read information now.
can i purchase cheap levaquin without a prescription
Get information now. drug information and news for professionals and consumers.
Get warning information here. All trends of medicament.
generic nexium online
Get information now. drug information and news for professionals and consumers.
drug information and news for professionals and consumers. Top 100 Searched Drugs.
https://nexium.top/# how to buy generic nexium online
Medscape Drugs & Diseases. Medscape Drugs & Diseases.
Best and news about drug. drug information and news for professionals and consumers. https://avodart.science/# buy avodart without a prescription
Drug information. п»їMedicament prescribing information.
All trends of medicament. Comprehensive side effect and adverse reaction information. https://avodart.science/# where can i get cheap avodart prices
Read information now. Top 100 Searched Drugs.
To the aiiore.com owner, Thanks for the well-written and informative post!
Dear aiiore.com admin, Your posts are always a great source of knowledge.
Comprehensive side effect and adverse reaction information. Actual trends of drug.
how to buy mobic no prescription
Read information now. Long-Term Effects.
drug information and news for professionals and consumers. Commonly Used Drugs Charts.
where to get generic mobic pill
Actual trends of drug. Some are medicines that help people when doctors prescribe.
Comprehensive side effect and adverse reaction information. Everything about medicine.
where can i get propecia for sale
Definitive journal of drugs and therapeutics. Everything what you want to know about pills.
Prescription Drug Information, Interactions & Side. Everything information about medication.
https://finasteridest.online where can i get generic propecia price
Long-Term Effects. Generic Name.
melbet promo code Click Here: https://www.nationallobsterhatchery.co.uk/news/melbet_promo_code__sign_up_offer.html
Get warning information here. Definitive journal of drugs and therapeutics.
https://finasteridest.com/ can i purchase propecia
All trends of medicament. Drugs information sheet.
Definitive journal of drugs and therapeutics. Long-Term Effects.
generic zithromax 500mg
Read information now. Read now.
how do i get 1xbet promo code Click Here: https://www.lafp.org/includes/pages/1xbet-promo-code-1xbet-bonus.html
промокод в мелбет Click Here: https://caravela.coffee/pages/promokod_melbet_pri_registracii_na_pervuy_depozit.html
Get warning information here. Everything information about medication.
where to buy cheap propecia pills
What side effects can this medication cause? Read information now.
Actual trends of drug. Medscape Drugs & Diseases.
https://clomiphenes.com can i get clomid prices
Generic Name. Top 100 Searched Drugs.
Dear aiiore.com owner, Thanks for the well-researched and well-written post!
Hello aiiore.com owner, Great content!
Read information now. What side effects can this medication cause?
https://azithromycins.com/ where can i buy zithromax in canada
Everything information about medication. Cautions.
Commonly Used Drugs Charts. Definitive journal of drugs and therapeutics.
zithromax buy online
Drugs information sheet. drug information and news for professionals and consumers.
Learn about the side effects, dosages, and interactions. What side effects can this medication cause?
https://finasteridest.com/ can i get cheap propecia no prescription
Generic Name. Everything what you want to know about pills.
drug information and news for professionals and consumers. Cautions. where can you buy amoxicillin over the counter
Get warning information here. Drugs information sheet.
Top 100 Searched Drugs. Read information now.
https://clomiphenes.com can i get generic clomid online
drug information and news for professionals and consumers. Read now.
Drug information. Everything what you want to know about pills.
get generic clomid without prescription
earch our drug database. Prescription Drug Information, Interactions & Side.
Top 100 Searched Drugs. drug information and news for professionals and consumers.
https://clomiphenes.com cost of cheap clomid pill
Some trends of drugs. What side effects can this medication cause?
Read information now. Get warning information here.
https://clomiphenes.com get generic clomid tablets
Definitive journal of drugs and therapeutics. Cautions.
Drugs information sheet. Definitive journal of drugs and therapeutics.
where can i buy cheap propecia for sale
Read now. drug information and news for professionals and consumers.
Drug information. What side effects can this medication cause? amoxicillin 1000 mg capsule
Read information now. Some are medicines that help people when doctors prescribe.
Read information now. Learn about the side effects, dosages, and interactions.
can you get cheap propecia price
Generic Name. earch our drug database.
Read now. Medscape Drugs & Diseases. where can i buy amoxicillin over the counter uk
earch our drug database. earch our drug database.
Learn about the side effects, dosages, and interactions. drug information and news for professionals and consumers. https://amoxicillins.online/ amoxicillin 500mg cost
Some trends of drugs. Learn about the side effects, dosages, and interactions.
drug information and news for professionals and consumers. Read here.
buy cheap zithromax online
Read here. Read information now.
Drug information. Drug information.
pills erectile dysfunction
Get warning information here. Learn about the side effects, dosages, and interactions.
What side effects can this medication cause? Medscape Drugs & Diseases.
https://edonlinefast.com cheap erectile dysfunction pills online
Some are medicines that help people when doctors prescribe. Read here.
Cautions. Actual trends of drug.
ed pills gnc
All trends of medicament. п»їMedicament prescribing information.
Everything information about medication. Read here.
ed pills cheap
What side effects can this medication cause? Everything information about medication.
Commonly Used Drugs Charts. п»їMedicament prescribing information.
the best ed pill
Comprehensive side effect and adverse reaction information. Everything what you want to know about pills.
Some are medicines that help people when doctors prescribe. earch our drug database.
best medication for ed
Medscape Drugs & Diseases. Get here.
Learn about the side effects, dosages, and interactions. Actual trends of drug.
ed treatments
Drug information. Everything information about medication.
Some trends of drugs. Actual trends of drug.
https://edonlinefast.com best ed treatment
п»їMedicament prescribing information. Read now.
Long-Term Effects. safe and effective drugs are available.
https://clomiphenes.online can i buy generic clomid without a prescription
Cautions. All trends of medicament.
Cautions. Some trends of drugs.
best ed pills non prescription
Prescription Drug Information, Interactions & Side. Medscape Drugs & Diseases.
п»їMedicament prescribing information. Generic Name.
canadian pharmacy cialis 20mg
earch our drug database. Best and news about drug.
Everything about medicine. Read information now.
pharmacy com canada
Everything what you want to know about pills. Commonly Used Drugs Charts.
Medscape Drugs & Diseases. Long-Term Effects.
best ed pills non prescription
What side effects can this medication cause? safe and effective drugs are available.
All trends of medicament. Read information now.
pet antibiotics without vet prescription
Generic Name. safe and effective drugs are available.
Cautions. What side effects can this medication cause?
https://canadianfast.online/# buy prescription drugs without doctor
Actual trends of drug. Get information now.
Get warning information here. Some trends of drugs.
canadian pharmacy 24h com
Read information now. safe and effective drugs are available.
Definitive journal of drugs and therapeutics. Get information now.
how can i order prescription drugs without a doctor
Commonly Used Drugs Charts. Read information now.
What side effects can this medication cause? Commonly Used Drugs Charts.
canadian pharmacy reviews
Read here. Drugs information sheet.
All trends of medicament. Some are medicines that help people when doctors prescribe.
https://canadianfast.online/# comfortis without vet prescription
Some are medicines that help people when doctors prescribe. Read now.
Long-Term Effects. Drug information.
https://canadianfast.online/# best online canadian pharmacy
Read now. safe and effective drugs are available.
Everything information about medication. All trends of medicament.
buy prescription drugs from canada cheap
Long-Term Effects. Everything about medicine.
safe and effective drugs are available. Get here.
non prescription erection pills
Drug information. Comprehensive side effect and adverse reaction information.
Everything about medicine. What side effects can this medication cause?
https://canadianfast.com/# pet meds without vet prescription canada
Read information now. Read here.
Some trends of drugs. Actual trends of drug.
https://canadianfast.com/# ed meds online without prescription or membership
Cautions. Long-Term Effects.
Dear aiiore.com administrator, Your posts are always well-cited and reliable.
Dear aiiore.com administrator, Your posts are always on topic and relevant.
Hello aiiore.com webmaster, Thanks for the well-organized and comprehensive post!
Learn about the side effects, dosages, and interactions. earch our drug database.
cost of sildenafil 20 mg
Cautions. Get warning information here.
Read information now. Some are medicines that help people when doctors prescribe.
sildenafil online sale
Read now. safe and effective drugs are available.
Read information now. Everything what you want to know about pills.
100mg sildenafil coupon
Everything information about medication. Everything what you want to know about pills.
safe and effective drugs are available. All trends of medicament.
sildenafil otc nz
Read here. Some are medicines that help people when doctors prescribe.
Some are medicines that help people when doctors prescribe. Prescription Drug Information, Interactions & Side.
sildenafil buy from canada
Get information now. Commonly Used Drugs Charts.
Some trends of drugs. Get here.
viagra professional uk
Learn about the side effects, dosages, and interactions. Medscape Drugs & Diseases.
Hello aiiore.com admin, Thanks for the informative and well-written post!
Everything about medicine. Long-Term Effects.
sildenafil 20 mg coupon
Top 100 Searched Drugs. п»їMedicament prescribing information.
What side effects can this medication cause? Read now.
https://tadalafil1st.com/# cialis online overnight delivery
Drug information. Medscape Drugs & Diseases.
Definitive journal of drugs and therapeutics. Commonly Used Drugs Charts.
canadian online pharmacy tadalafil
Long-Term Effects. earch our drug database.
п»їMedicament prescribing information. safe and effective drugs are available.
cialis without rx
Top 100 Searched Drugs. Actual trends of drug.
Drug information. All trends of medicament.
tadalafil 2
Best and news about drug. Drugs information sheet.
Hello aiiore.com admin, Keep up the great work!
Medscape Drugs & Diseases. п»їMedicament prescribing information.
cheapest generic cialis online
Learn about the side effects, dosages, and interactions. Learn about the side effects, dosages, and interactions.
Gabung slot online Dewapoker bisa JP klo main di sana, member baru di manjain banget soalnya jadi gak takut rungkad. Situs slot gacor resmi gampang menang dilengkapi dengan bocoran link judi slot terpercaya serta rtp tinggi cukup hanya dengan dana 10k anda bisa bermain slot online naga poker pasti mudah maxwin. Jadi, tidak perlu ragu lagi untuk memainkan game provider judi slot online yang terbaik bernama Dewapoker.
Generic Name. Long-Term Effects.
36 hour cialis
Everything what you want to know about pills. Everything about medicine.
Read here. Drugs information sheet.
generic cialis tadalafil uk
Read information now. Cautions.
Dear aiiore.com webmaster, Your posts are always well-referenced and credible.
Hi aiiore.com admin, Excellent work!
Get information now. Read here.
https://tadalafil1st.com/# buy cialis in australia online
Commonly Used Drugs Charts. Best and news about drug.
Definitive journal of drugs and therapeutics. drug information and news for professionals and consumers.
https://tadalafil1st.online/# 20 mg cialis vs 100mg viagra
earch our drug database. Everything information about medication.
Drug information. Cautions.
cheapest tadalafil india
Actual trends of drug. Everything what you want to know about pills.
Cautions. Everything information about medication.
overnight cialis online
Cautions. Learn about the side effects, dosages, and interactions.
Actual trends of drug. Read information now.
cialis mastercard
Drugs information sheet. Read now.
Get information now. Everything information about medication.
pay cialis with pay pal
Everything about medicine. Some trends of drugs.
Actual trends of drug. Some trends of drugs.
https://tadalafil1st.com/# buy tadalafil online paypal
Read information now. Prescription Drug Information, Interactions & Side.
Long-Term Effects. п»їMedicament prescribing information.
prednisone without rx
Everything information about medication. Everything about medicine.
To the aiiore.com webmaster, Thanks for the well-researched post!
Dear aiiore.com webmaster, You always provide valuable feedback and suggestions.
Very nice post. I just stumbled upon your blog and wanted to say that I’ve really enjoyed browsing your blog posts. In any case I’ll be subscribing to your feed and I hope you write again soon!
Very nice post. I just stumbled upon your blog and wanted to say that I’ve really enjoyed browsing your blog posts. In any case I’ll be subscribing to your feed and I hope you write again soon!
Get warning information here. Read here.
https://propeciaf.store/ order cheap propecia
Cautions. Generic Name.
Hello aiiore.com admin, Thanks for the great post!
The unfortunate truth is that, for most women, very little can be done to prevent breast cancer is cialis generic
Best and news about drug. Read information now.
https://propeciaf.store/ how to get cheap propecia without a prescription
Some are medicines that help people when doctors prescribe. What side effects can this medication cause?
Definitive journal of drugs and therapeutics. Prescription Drug Information, Interactions & Side.
how to buy propecia prices
Actual trends of drug. Prescription Drug Information, Interactions & Side.
To the aiiore.com admin, Excellent work!
Cool. I spent a long time looking for relevant content and found that your article gave me new ideas, which is very helpful for my research. I think my thesis can be completed more smoothly. Thank you.
Cool. I spent a long time looking for relevant content and found that your article gave me new ideas, which is very helpful for my research. I think my thesis can be completed more smoothly. Thank you.
Hi aiiore.com owner, You always provide key takeaways and summaries.
Hi aiiore.com webmaster, Thanks for the informative post!
To the aiiore.com administrator, Thanks for the informative and well-written post!
Hi aiiore.com owner, Your posts are always well structured and easy to follow.
Hi aiiore.com owner, Thanks for the valuable information!
Hello aiiore.com webmaster, Your posts are always well-supported by research and data.
To the aiiore.com webmaster, You always provide useful tips and best practices.
An impressive share, I just given this onto a colleague who was doing a little analysis on this. And he in fact bought me breakfast because I found it for him.. smile. So let me reword that: Thnx for the treat! But yeah Thnkx for spending the time to discuss this, I feel strongly about it and love reading more on this topic. If possible, as you become expertise, would you mind updating your blog with more details? It is highly helpful for me. Big thumb up for this blog post!