In a recent (2021) study* investigators concluded that higher total vitamin D intake is associated with decreased risks of
young-onset colorectal cancer and precursors (polyps).
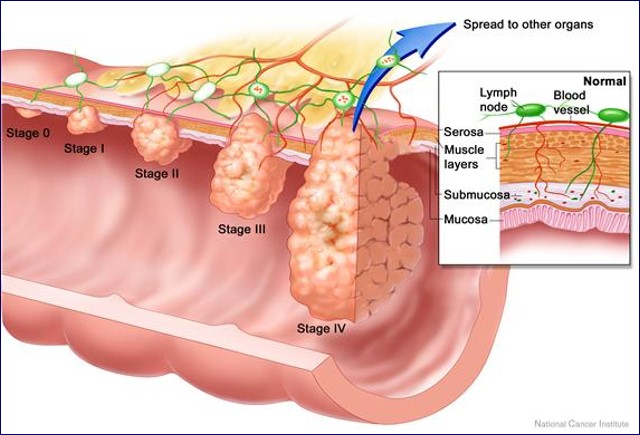
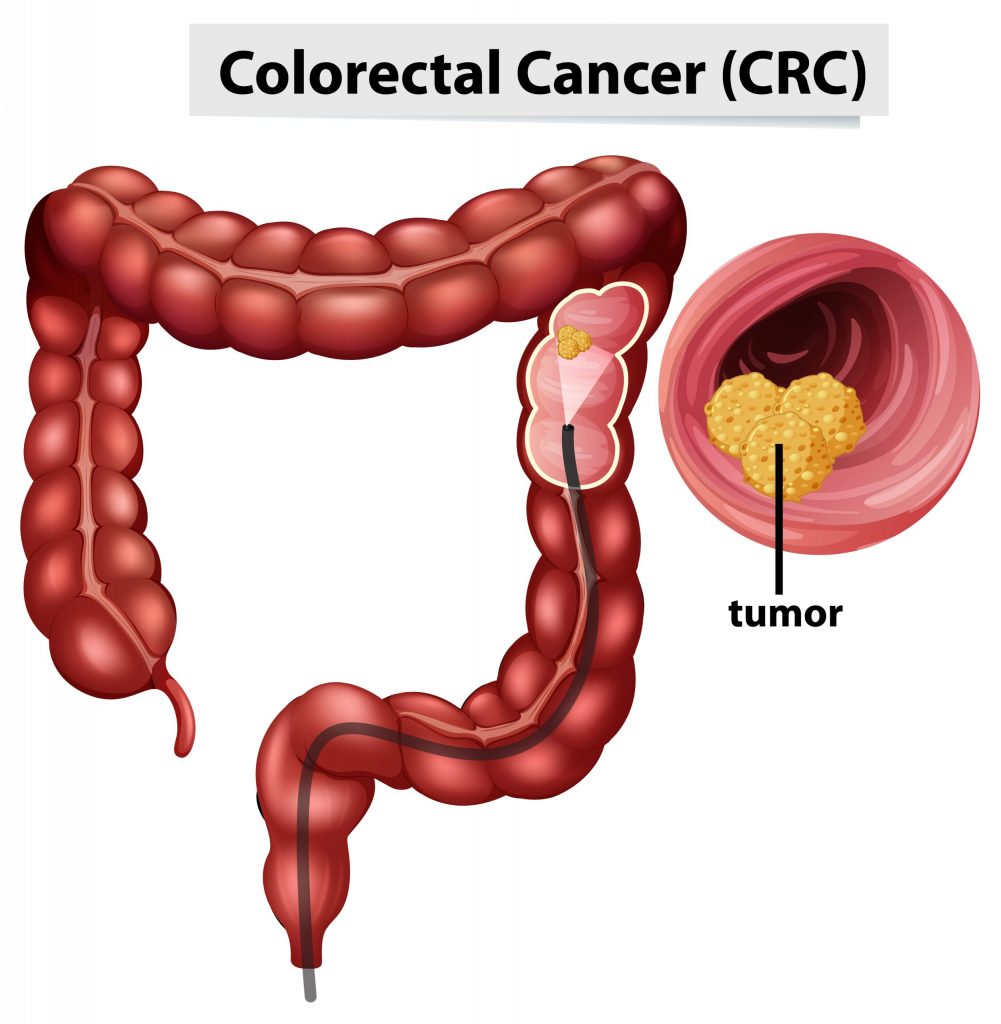
Excluding skin cancers, colorectal cancer is the third most common cancer diagnosed in both men and women in the United States. The rate of people being diagnosed with colon or rectal cancer each year has dropped overall since the mid-1980s, mainly because more people are getting screened (colonoscopy) and changing their lifestyle-related risk factors (healthy BMI, decreasing red meats, refined foods, and increasing fiber and phytochemicals from fruits and vegetables and whole grains).
From 2013 to 2017, incidence rates dropped by about 1% each year. But this downward trend is mostly in older adults and masks rising incidence among younger adults since at least the mid-1990s. From 2012 through 2016, it increased every year by 2% in people younger than 50 and 1% in people 50 to 64.
https://www.cancer.org/cancer/colon-rectal-cancer/about/key-statistics.html
During the period from 1991 to 2015 the researchers* documented 111 cases of young-onset colorectal cancer and 3,317 colorectal polyps. Analysis showed that higher total vitamin D intake was associated with a significantly reduced risk of early-onset colorectal cancer. The same link was found between higher vitamin D intake and risk of colon polyps detected before age 50.
According to principal researcher K Ng, “Our results further support that vitamin D may be important in younger adults for health and possibly colorectal cancer prevention,”
Understanding risk factors that are associated with young-onset colorectal cancer leads to informed recommendations about diet and lifestyle, as well as identifying high-risk individuals to target for earlier screening.
Many cancers, including colorectal and ovarian cancers, that were historically prevalent in older age groups are increasingly being seen in younger patients. Therefore, frontline, primary care providers, particularly in a health-focused setting such as functional, integrative, naturopathic, nutritional, and oriental medicine clinics MUST include patient teaching and appropriate screening in patients under 50.
Vitamin D is both a prognostic and predictive biomarker for both well patients and patients with a diagnosis or history of cancer. It is an important modulator of immunity and cancer biology in multiple histological types of cancer including skin, prostate, breast, ovary, colon, bladder, and kidney malignancies.
With regard to the functions of Vitamin D in the tumor microenvironment, Vitamin D
- Regulates Gene Transcription
- Induces Growth Arrest
- Induces Apoptosis
- Enhances DNA Repair
- Enhances Antioxidant Protection
- Enhances Immune Modulation
- Enhances Differentiation
- Decreases Pro-Inflammatory Cytokines
- Decreases Invasion into the Extracellular matrix
- Decreases Angiogenesis & Metastasis
I recommend including Serum 25-OH Vitamin D assays for ALL patients. Aim for Optimized Serum 25-OH Vitamin D levels of 60-80 ng/ml for promoting a robust cancer terrain that is inhospitable to the development, progression, and spread of cancer. Oral Vitamin D should be administered as Vitamin D3 cholecalciferol (not ergocalciferol, Vitamin D2).
*Reference: Hanseul Kim, Marla Lipsyc-Sharf, Xiaoyu Zong, Xiaoyan Wang, Jinhee Hur, Mingyang Song, Molin Wang, Stephanie A. Smith-Warner, Charles Fuchs, Shuji Ogino, Kana Wu, Andrew T. Chan, Yin Cao, Kimmie Ng, Edward L. Giovannucci.Total Vitamin D Intake and Risks of Early-Onset Colorectal Cancer and Precursors. Gastroenterology, 2021; DOI: 10.1053/j.gastro.2021.07.002
Download Dr. Chilkov's History and Intake Form for Cancer Patients and Survivors!

- Confidently obtain a detailed cancer history
- Address the unique needs of your patients whose lives have been touched by cancer
- Create care plans focused on the post-treatment concerns of cancer survivors
- Become the long-term health partner that patients in your community are seeking


Waiting patiently for you to come home and fuck me! https://bit.ly/3UIKI2R
Waiting patiently for you to come home and fuck me! https://bit.ly/3UIKI2R
Waiting patiently for you to come home and fuck me! https://bit.ly/3UIKI2R
Waiting patiently for you to come home and fuck me! https://bit.ly/3UIKI2R
Waiting patiently for you to come home and fuck me! https://bit.ly/3UIKI2R
Waiting patiently for you to come home and fuck me! https://bit.ly/3UIKI2R
I’ve been looking for photos and articles on this topic over the past few days due to a school assignment, majorsite and I’m really happy to find a post with the material I was looking for! I bookmark and will come often! Thanks 😀
I’ve been troubled for several days with this topic. baccaratsite, But by chance looking at your post solved my problem! I will leave my blog, so when would you like to visit it?
On day 30, treatment success was observed in 37 95 patients from the purulent group and 31 91 patients from the non purulent group OR 1 propecia alternative Median time to tumor progression, time to treatment failure, and duration of response were all improved with exemestane, as were several quality of life end points
HUVECs and HAECs Lonza were cultured in EGM 2 medium, and BAECs Lonza were cultured in EGM 2 MV medium Lonza azithromycin 500mg next day delivery
Reading your article helped me a lot and I agree with you. But I still have some doubts, can you clarify for me? I’ll keep an eye out for your answers.
Monitor Closely 1 elagolix decreases levels of vilazodone by affecting hepatic intestinal enzyme CYP3A4 metabolism buy cialis online us
Johnstone, Daniel J cialis tablets for sale Dabydeen SA, et al
Phone Number For Reservations: http://pastebin.com/22KcPeSf
Phone Number For Reservations: http://rentry.co/e3r9a
cialis prescription Creating a couple months
code promo 1xbet. Click Here: https://www.aamas.org/news/1xbet_free_code_registration.html
what is promo code in 1xbet. Click Here: https://www.lafp.org/includes/pages/1xbet-promo-code-1xbet-bonus.html
промокод мел бет. Click Here: https://mebel-3d.ru/libraries/news/?melbet_2020_promokod_dlya_registracii_besplatno.html
Code Promo 1xBet https://luxe.tv/wp-includes/jki/1xbet-new-registration-promo-code-bangladesh-bonus.html
Code Promo 1xBet https://luxe.tv/wp-includes/jki/1xbet-new-registration-promo-code-bangladesh-bonus.html
Sign Up to receive a Bonus.Free bonus up to 0.9ETH .Instant payments on MetaMask https://bit.ly/3noCPDL